Insights for Sales Leaders
Best practices, industry trends, and strategies to optimize your call center operations
Customer Story
Apr 16, 2026
2 min read
How Century Benefits Tested Onyx With One Team Before Moving Their Entire Agency
Switching platforms is a big decision. You're betting your operation on software you haven't fully stress-tested, asking your team to learn new workflows, and hoping nothing breaks along the way.
Andrew Eachon, owner of Century Benefits, wasn't willing to take that bet all at once. So he didn't.
Starting Small With One Team
Century Benefits runs multiple agent teams remotely and out of offices in Portland and Vancouver. When Eachon started evaluating Onyx Platform, he saw an opportunity to test without disrupting his core operation. Rather than migrating everyone at once, he brought a single sales team on first.
That team was already managing their own workflows and had flexibility in how they operated. It was a chance to see how the platform performed in real conditions, with real calls and real compliance requirements, before making a bigger commitment.
If Onyx delivered, he'd have months of real data to justify moving the rest of the agency. If it didn't, the core operation would keep running without interruption.
Five months later, the data was clear.
What Five Months Revealed
The improvements showed up in day-to-day workflows and overall performance. On Onyx, customer information loaded automatically when a call connected. Scripts appeared based on what the agent was selling. When a policy came through from Sunfire, the enrollment data pre-populated so agents could review and submit in a few clicks instead of rebuilding the record from scratch. After-call notes wrote themselves.
The platform also gave sales managers a cleaner view of performance. Eachon's team worked with Onyx to customize their scoreboard to show only what mattered: inbound calls taken, policies sold, closing percentage, and billable hours. Five data points on a TV screen, refreshing every 15 minutes.
None of this was theoretical anymore. Eachon had months of real performance data from agents doing real work.
Moving the Whole Agency
After the pilot, moving the whole agency felt obvious.
The risk that made Eachon hesitant in the first place had been tested and answered. He knew how onboarding worked because he'd already done it. He knew which questions agents would ask because the initial team had already asked them. He knew what training looked like and how long it took for people to get comfortable.
Century Benefits brought everyone on in early 2026. The agency's operations manager handled the rollout from one of their offices. On launch day, only a handful of last-minute questions came up. "Pretty smooth, everybody's happy," they told the Onyx team on their daily checkin call.
Read Article
More Articles

Insight
The 5-Tool Problem: How Technology Slows Your Agency Down
Most insurance agencies we talk to are running five or six disconnected platforms: a CRM that doesn’t know what happened in the dialer, a compliance system that generates reports nobody reads, and reporting stitched together by hand. Every new tool promises efficiency. Too often, it makes the agency slower.
Five Logins Before the First Call
We hear it on nearly every demo. One agency owner described his tech stack as “madness”: six platforms, huge combined bills, and agents context-switching after every call. His team wasn’t selling more. They were navigating more.
Another agency told us their CRM and dialer technically coexisted, but “there’s just some weird stuff in the way they connect.” To get a unified view of the business, the ops team built custom tooling to combine what should have already been one dataset.
That’s the tax nobody budgets for. Not the seat fee. Not the cost per minute. The human cost of holding the stack together by hand.
And the more you grow, the worse it gets. New agents learn five workflows instead of one. Managers pull numbers from three places to answer one question. Compliance reviews mean reconciling recordings, lead records, and timestamps and hoping everything lines up.
Adding a Tool Makes it Worse
When something breaks, the instinct is to buy another tool. A QA platform. An AI scoring add-on. A sync layer between the CRM and the dialer. But every new integration adds another seam, and seams are where things fall apart.
Take compliance scoring. The dialer records the call. Another system transcribes it. A third scores it. The results land in a dashboard disconnected from everything else. Now a manager wants to know whether compliance issues are hurting conversion. The answer lives across three platforms, so the question often never gets answered.
That’s the real cost: not the integration fee, but the questions your team stops asking because the data is too scattered to answer.
One System That Learns From Itself
When the dialer, CRM, compliance engine, and routing logic share one data layer, each action informs the next. Calls get scored in real time. Records update immediately. Follow-up tasks carry the right context. Routing reflects live data, not stale exports.
None of this requires another integration. It’s what happens when the data already lives in one place.

Perspective
What "AI-Powered" Should Mean for Insurance Agencies and the Insurance Market
There is a lot of "AI-powered" software in insurance right now, and a lot of it feels like the same pitch with different branding.
Add a chatbot. Add a note summary. Add a score. Add a copilot button. Add another tool. Hope your team uses it.
We think that is backwards.
If you run an agency or carrier operation in a regulated market, the question is not whether AI is exciting. The question is whether it helps your business work better on real days, with real agents, real members, real policies, and real compliance requirements on the line.
That starts with a simple truth: organizations do not adopt AI in the same way, and they do not all want software to work the same way either.
The right AI depends on how your team wants to work
Most of the industry puts agencies on a single spectrum from "getting started with AI" to "advanced AI team." That misses something important. A 500-seat call center with a sharp ops team might configure every routing rule, scoring threshold, and automation trigger on the platform, and never once talk to an AI. Under the single-spectrum model, they look like beginners. They are not. They just want AI to be invisible.
We think about AI in insurance and agency operations along two independent dimensions.
AI visibility: is AI invisible or fully interactive? On one end, AI works behind the scenes. It scores calls, ranks lead sources, flags compliance issues. Your team never interacts with it. On the other end, AI is something your team talks to. They ask questions, trigger actions, get answers.
Solution usage style: does your team take the defaults, or configure the system? Some teams want strong out-of-the-box experiences. Others want to design the rules, set the thresholds, and build workflows that match how their operation actually runs.
Those two dimensions create four identities.
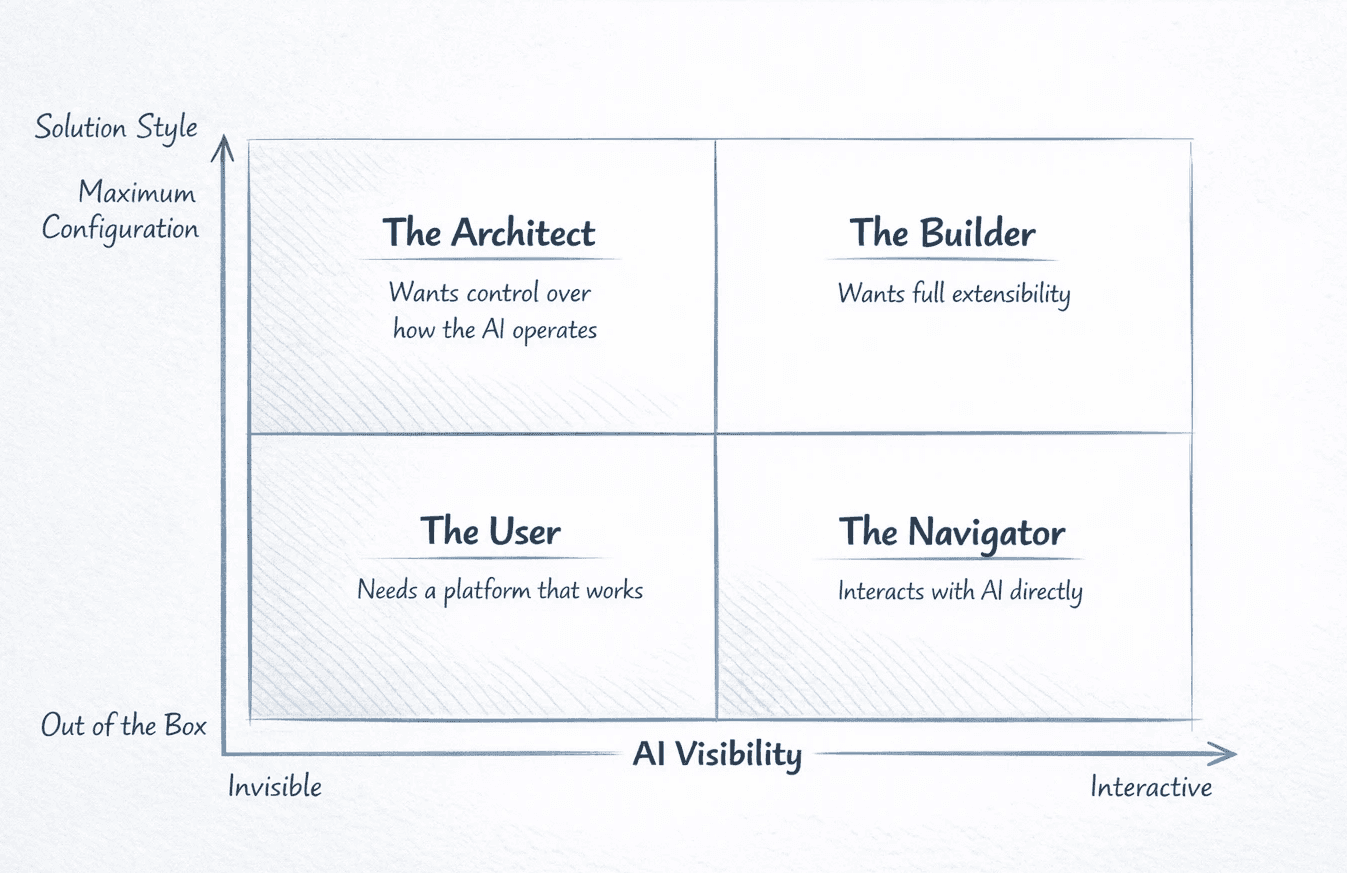
The User does not think about AI. Compliance scoring runs automatically. Lead sources get ranked. Coaching flags show up. No settings page, just results. This is where most people inside an agency are: the agent making calls, the manager reviewing performance, the coordinator scheduling follow-ups. They do not need a relationship with AI. They need a platform that works.
The Navigator interacts with AI directly, but through served experiences. They ask the assistant about yesterday's call volume. They pull a report without building one. They get an answer from operational data without filing a ticket. The AI is visible and useful, but the Navigator is not configuring anything.
The Architect wants control over how AI operates. They design the scoring criteria, the routing logic, the coaching thresholds, the automation rules. Then they walk away and let the system execute. Platform power users, not AI power users.
The Builder wants full extensibility. They connect Claude, Manus, or custom tools to the platform via MCP and SDK. They build workflows that span multiple systems.
What matters is that these are not fixed labels.
Over time, nearly every agency will adopt AI in some form. What changes is how people want to use it. Some teams will start as Users and grow into Navigators or Architects. A smaller group will become Builders. And as the platform evolves, what requires a Builder today becomes accessible to a User tomorrow.
That pattern is not unique to AI. In enterprise software, there have always been teams that want strong defaults and teams that want more control. We expect the AI axis to move over time. We do not expect that core difference in usage style to disappear.
Our job is to be there for all styles today and support their journeys over the next few months and years.
AI only works if it sits on top of a real operating system
This is where a lot of AI products break down.
They can generate something interesting, but they are disconnected from the real operating system of the business. They do not understand the lead, the policy, the agent, the compliance workflow, or what happened on the last call. They are a layer, or a point solution, not a system.
That is not enough for insurance.
If AI is going to improve outcomes in a compliant and durable way, it has to sit on top of a platform that already understands the business. Every lead. Every policy. Every agent. Every call. Every compliance event. Every handoff.
That is how AI stops being a demo feature and starts becoming operational leverage.
A voice bot can only route well if it understands context and downstream ownership. A compliance reviewer is only useful if its output ties back to real workflows managers can act on. An SMS reviewer only matters if it is connected to the actual conversation history, permissions, and recordkeeping underneath it. An assistant only helps if it can answer questions from the real system your team runs on.
This is also why we think agencies and carriers should not have to choose between safe and useful. If the platform underneath is strong, you can have both.
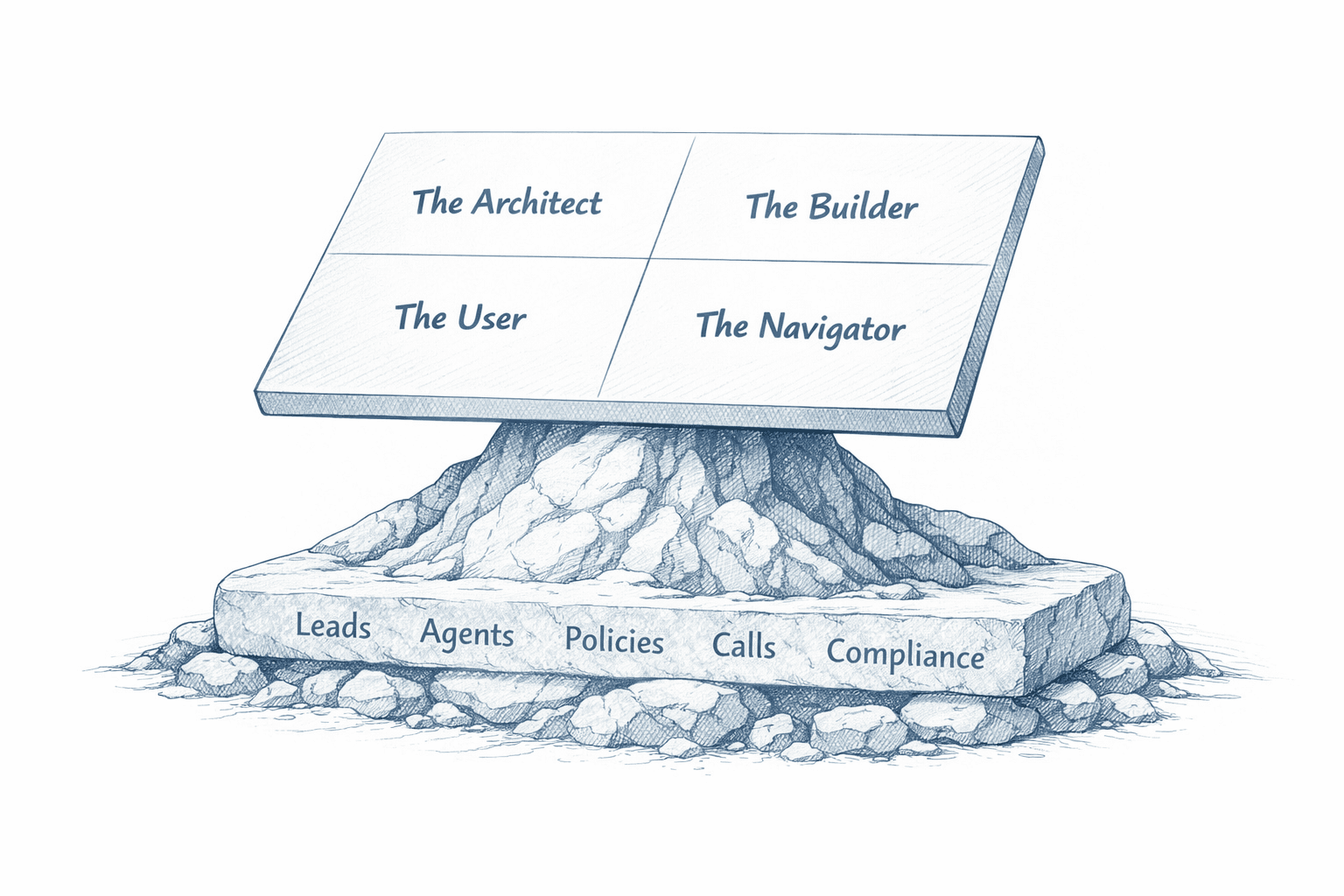
AI should make the business better, not just make the product sound modern
We are building AI across that full spectrum. But the goal is not to shove AI into every corner of the product and hope customers adapt.
The goal is to help agencies and carriers get stronger in ways that actually matter. Better compliance. Faster decisions. Better coaching. Better use of agent time. Better follow-up. Better transfer logic. Better visibility.
Some customers want one strong default. Some want configurable systems. Some want to build with us. We are here for all of them, and for the teams that will move between them over time.
That is what "AI-powered" should mean: not more noise, not more disconnected features, but better business outcomes built on top of a platform that already knows how your operation works.

Perspective
Your Best Clients Are the Ones You Can't Reach by Phone
This is the reality of busy clients. They're picking up grandkids from school, getting to a physical therapy appointment, helping a neighbor with groceries, or finishing some garden work while the light's good. They still need coverage, and the coverage they need is often complicated: three specialists to keep, a drug list that has to line up, a spouse on a different plan. They're not avoiding the decision. They just have a whole life happening around it.
What they want is an agent they trust. Someone they can fire a quick text to with a question. Someone who texts back like a real person. Once they have that, they stay. That relationship is what turns a single enrollment into a client who renews year after year.
Phone-Only Loses the People Who Matter Most
The hard cases don't fit inside a single call, and a phone-only workflow turns them into phone tag. Your agent calls. Straight to voicemail. The member calls back while the agent is on another line. By the time they finally reconnect, the moment has passed, the kitchen table is covered in mail from competitors, and a member who would have been loyal for years drifts to whoever caught them at the right minute.
The agent didn't do anything wrong. The channel did. Phone calls are synchronous and life is not. Every missed connection is a round where the relationship isn't building, and on complex cases, that relationship is what decides whether the policy gets written and whether it sticks at next AEP.
What Texting Looks Like in a Real Case
Here's the same situation handled over text, between dials. The agent is on calls all afternoon. The member is out running errands. The thread might look like this:
Agent: Take your time. I'm waiting on a callback from Dr. Chen's office around 1pm to confirm she's in network. I already found her listed online but I want to double-check, I know how important she is to you.
Member: OK I'm out at the playground, I'll check my phone every 30 or 40 minutes. Just text me when you have an answer.
Agent: Hey, still working on it, should be soon. Sorry it's taking a bit, I'll text you the moment everything's confirmed.
Member: No rush, take the time you need. I really appreciate you checking.
Agent: All confirmed, she's in network. Want me to call you in the morning to walk through the plan and get you enrolled?
Member: Yes, 10am works. Thank you for being so kind.
Nothing dramatic happened. That's the point. The agent kept eight conversations like this alive in parallel between live dials, the member felt cared for instead of chased, and a complex case that would have died in voicemail closed the next morning.
The real payoff is what comes after. The number the member texted at enrollment is the same number they text when their drug gets dropped from formulary, when a confusing letter arrives from CMS, when a friend asks for a referral. The agent becomes their person. That's how a book of business compounds instead of churns.
How Onyx Texting Works
Onyx texting runs from an agent’s number tied to your agency, not their personal cell. Every message is logged against the member's record, so the relationship history is always there. Consent is captured live on the call through a built-in script before any text goes out, stored with a timestamp tied back to that call. If a member ever wants out, they reply STOP and Onyx handles the opt-out automatically. Your agents stay focused on the conversation. The compliance plumbing runs underneath.
The Bottom Line
Busy seniors with complicated needs are exactly the people who reward a trusted agent with years of loyalty. Give your agents a channel that fits the gaps in someone's day, and the retention builds itself.

Customer Story
More Applications, Fewer Hours: How A+ Insurance Designers Grew Agent Output with Onyx Platform
A+ Insurance Designers is a Dallas-based FMO founded in 2013. They partner with licensed agents nationwide to sell ACA marketplace plans across multiple carriers. What makes their operation distinct is who they serve: a large share of their clients speak English as a second language and are navigating the marketplace for the first time.
That shapes everything about how A+ runs. Their agents don't just sell. They explain plan options in someone's first language, handle customer care calls about payment failures and renewals in that language, and switch between sales and service throughout the day. When every agent is doing double duty, every hour of workflow friction compounds across the entire operation.
After running with Onyx Platform through their most recent Open Enrollment Period (OEP), the A+ team measured the difference:
Applications per agent increased +12.5%
Members per agent increased +13.3%
Hours per application decreased -14.3%
Onyx has helped us increase applications per agent by 12.5% and members per agent by 13.3%. We're able to effectively manage a growing client base with greater operational efficiency. Hours per application decreased by 14.3% compared to the previous Open Enrollment Period. Onyx enables us to work smarter.
Carson Choate, CEO of A+ Insurance Designers
One System Replaced Five Workflows
Before Onyx, A+ ran on a separate CRM, a separate dialer, and HealthSherpa for policy submissions. Agents toggled between systems to look up a customer, check a policy, make a call, and log the outcome. Every handoff was lost time.
When A+ moved to Onyx, their operations department flagged a field that most CRMs don't support natively: a language tag on every customer record. For A+, that's not metadata. It's how they route work. If an agent doesn't know whether to greet someone in a specific language before the call connects, the conversation starts wrong.
Onyx brought that language data in and made it searchable and filterable. The dialer, CRM, scripting, and lead management now live in one platform. When an agent picks up a call, the customer's history, policies, and language preference are already on screen. After-call logging happens automatically. Scripts are intentionally lightweight, structured guidelines rather than rigid talk tracks, because multilingual agents need flexibility to have natural conversations. That's how hours per application drops 14% without anyone changing how they sell.
Onyx Platform also auto-detects which language a call is in and transcribes it in the correct language. For a multilingual agency, that means every call is documented accurately regardless of which language it was conducted in, without anyone doing extra work.
Missed Calls Became the Second Pipeline
Most agencies treat missed inbound calls as lost. At A+, Onyx's task system automatically creates a follow-up when a call goes unanswered, surfaced in the same workspace the agent already uses, attached to the full customer record.
The results: A+ agents complete callback follow-up tasks at a rate above 95%. Many of these callbacks convert into policies. Their recovery rate comes from eliminating the friction between "missed call" and "callback": no separate voicemail queue, no spreadsheet, no context switching. The task appears with full history, and picking up the thread takes seconds.
Efficiency Created Room to Grow
Carson Choate, CEO of A+ Insurance Designers, has since expanded the agency from purely ACA into Medicare Advantage enrollment through Onyx's HealthSherpa integration.
If your agency is growing and your per-agent numbers aren't keeping up, we should talk.

